Payer Influence On Product Performance in Pharm Industry
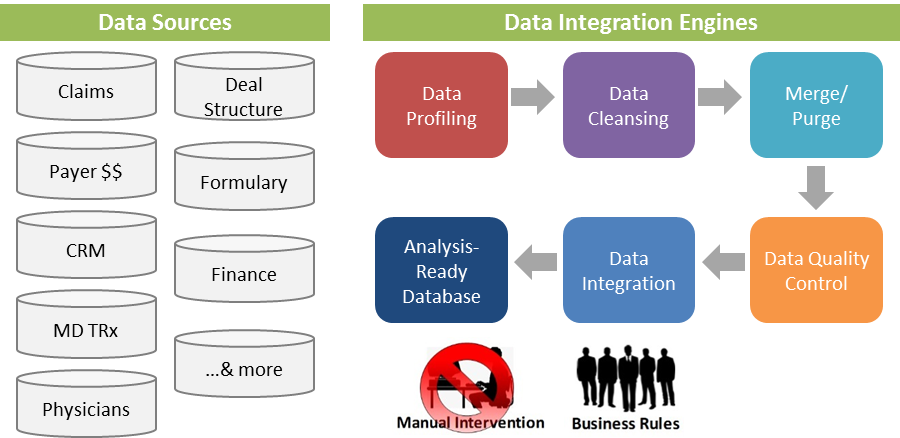
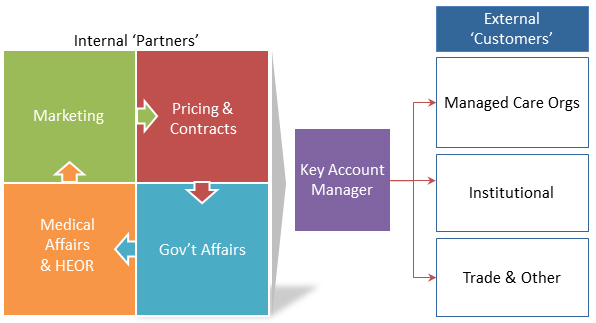
Payers vary in their ability to assert formulary compliance. We will explore how tools and analytics can enable a pharmaceutical manufacturer to assess factors impacting formulary control and incorporate those findings when evaluating contracting opportunities. We apply these approaches to understand the various levers payers use to control product utilization and measure the direct and indirect (“spillover”) impact they have on prescribing. “Levers” include various formulary access controls such as Prior Authorization, Step Edit, and Tier Position/Co-pay. A true understanding of these components can have profound implications on contracting terms and rebates, and actually extend to other areas such as targeting, incentive compensation, etc.
Contact us at insights@axtria.com with any questions.