As per a systemic review1 published in Annals of Internal Medicine, assessing the impact of interventions to improve adherence, it was found that about half the medications prescribed for chronic diseases are not consumed as directed by the physician, and around 20-30% of prescriptions are never fulfilled. This non-adherence results in over 125,000 deaths every year as well as increased emergency department visits and hospitalizations, which costs the American healthcare system to the tune of $100 to $300 billion1.
The reasons for lack of compliance to medication prescribed by their health care practitioners (HCPs), amongst others, are:
- The absence of knowledge on the medicine’s effect and its importance in keeping them healthy
- The fear of side effects
- Lack of immediate physiological effect when not taking the medication
- The inconvenience of sticking to a complicated schedule – or compliance related to scheduling
- Affordability and access or lack of information about an individual’s access and affordability, and
- The increasing societal pressure to do things naturally
Pharma companies have, in the past, used human intervention (including nurses, case managers, pharmacists, etc.) to improve adherence, which although effective, can be very expensive, thus limiting the reach. Phone reminders have also been successful to some extent but can be too generic, offering no personalization and an inability to ensure that the reminder resulted in adherence, leading to patients losing interest.
Learn More - "Humanizing The Artificial Intelligence Foundation For Success"
To address compliance concerns, organizations are looking into creative solutions utilizing artificial intelligence (AI) and machine learning (ML) to increase patient adherence. Some of the solutions that have shown results in this field, include:
- Chatbots: Conversational AI focused on medication adherence can build a personalized patient profile and engage with them to help stay on track with their daily medications. It also helps in answering patients’ questions related to the medication, and their understanding, and addresses their reasons for non-adherence.
Examples of such tools that are available for patients today include Roborto2 and Maxwell3.
 Learn More - How Healthcare AI Chatbots Are Transforming The Patient Journey
Learn More - How Healthcare AI Chatbots Are Transforming The Patient Journey .jpg?width=300&name=shutterstock_1089426038%20(1).jpg) Smart pills: These pills include ingestible bio-sensors that are embedded into the medicine, which, when consumed, get dissolved in the body and send a signal to the patient and HCP on their smartphone through a wearable patch.
Smart pills: These pills include ingestible bio-sensors that are embedded into the medicine, which, when consumed, get dissolved in the body and send a signal to the patient and HCP on their smartphone through a wearable patch.
The FDA approved one such drug, Abilify MyCite, in November 2017. This method only tracks medication adherence and does not send any reminders to patients.- Wrist band sensors: The unique motion of taking the drug out of its packaging and consuming it can be tracked and help track medication adherence. This is a non-intrusive method of monitoring and improving adherence where reminders are sent to patients when they’ve not consumed the medicine at the prescribed time.
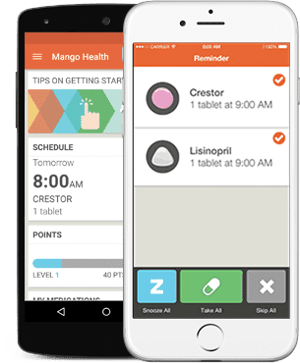 Gamification: Managing the disease and its side effects every day can become cumbersome, especially in the case of chronic diseases. Combining disease management with games can add an element of engagement and make routine tasks less boring. Such game-based apps aim to instill a behavior change in patients by rewarding them upon continued adherence, thus positively reinforcing right behaviors.
Gamification: Managing the disease and its side effects every day can become cumbersome, especially in the case of chronic diseases. Combining disease management with games can add an element of engagement and make routine tasks less boring. Such game-based apps aim to instill a behavior change in patients by rewarding them upon continued adherence, thus positively reinforcing right behaviors.
While using the Mango Health app, patients can earn the in-game currency upon adhering to medication schedule and level-up, which they can use to unlock real-life rewards. Bayer’s DIDGET blood glucose monitors, which are primarily used by children, can be connected with Nintendo gaming systems and award patients for good testing habits, which can be redeemed for new characters or costumes in the games.- Apps: There are multiple apps currently available on Apple (iOS) and Android OS to aid in improving patient adherence. These apps include features such as:
- time and dosage alerts
- tracking medication consumption
- refill reminders, and
- storage (of the medication) information.
Examples of such apps include Groove Health, AiCure, Medisafe, etc. - Smart packaging: There are pill dispensers available in which users can enter dosage and timing for medication and sync the device with the app on their smartphone. The device dispenses the required dosage at the predefined time while giving out an audio/visual signal to catch the patient’s attention. It also has the feature of alerting the caregiver/physician when the patient misses a dose. Some devices are voice-activated, giving the patient an option to chat with their caregiver. Smart bottles can track whether the patient has consumed the medicine through sensors in the cap (of the dispenser) which detect when the bottle is opened and through the weight of the remaining pills. High-tech versions of blister and strip packaging are also available, which follow the same principle of tracking when the medicine is removed. A drawback of the smart packaging is that the technology can track when a medicine is taken out of the packaging but not if it has been consumed.
A few examples of such products include Fellow Smart Pillbox, CleverCap that fits on standard pillboxes, sensors for inhalers by Propeller Health, and others.
AI and ML can also be used to predict patients at high risk of non-adherence. Certain factors are known to affect adherence such as zip code, diagnosis, the complexity of dosing regimen, ethnicity, employment status, patient age, gender, payer formulary status, insurance status, and medication cost. Data scientists can run analysis on available patient data utilizing this knowledge to classify patients into risk groups. Life sciences companies can then proactively intervene in cases of high-risk patients to ensure that they stay adherent. One can go a step further and integrate pharmacy retailers' point-of-sale (POS) data at the customer level from pharmacy retailers to create alerts for both patients and retailers, before an impending drug refill or even initiation of therapy, in certain cases. This will help bridge the last-mile gap from prescription to fulfillment.
![]() Download Case Study - Enabling 95% Patient Adherence With Rapid Patient Data Analytics
Download Case Study - Enabling 95% Patient Adherence With Rapid Patient Data Analytics
Of course, a major technology disclaimer is that for any measure aiming to improve adherence to be successful, the patient must be willing and motivated. Until that can be achieved, no matter how smart, the technology will not be able to force the patient to take the medication. The support network plays a vital role and must be tapped, especially in the case of chronic diseases, to ensure that the patient remains compliant. For younger patients, social media analysis can provide important insights on patient behavior. All stakeholders and touchpoints during a patient’s journey could play an important role in engaging the patient and ensuring compliance.
The use of AI and ML-powered digital tools is the next logical step in ensuring connected healthcare. Leveraging AI and ML to boost adherence can reduce the unnecessary burden on the healthcare system, improve patient outcomes, make clinical trial data more reliable, and impact pharma revenues.
![]() Click Here To Learn About Axtria's AI/ML Capabilities.
Click Here To Learn About Axtria's AI/ML Capabilities.
References
- Viswanathan M, Golin CE, Jones CD, et al. Interventions to Improve Adherence to Self-administered Medications for Chronic Diseases in the United States: A Systematic Review. Ann Intern Med, December 2012. Available at https://annals.org/aim/fullarticle/1357338/interventions-improve-adherence-self-administered-medications-chronic-diseases-united-states
- Fadhil A, A Conversational Interface to Improve Medication Adherence: Towards AI Support in Patient's Treatment, ResearchGate, March 2018, Available at https://www.researchgate.net/publication/324055736_A_Conversational_Interface_to_Improve_Medication_Adherence_Towards_AI_Support_in_Patient's_Treatment
- Groove Health website. Accessed in February 2020, Available at https://www.groovehealthrx.com/



